Dr. Lydia Buzaalirwa, the Senior Director for Quality Management and Medical Logistics at the AIDS Healthcare Foundation (AHF) Africa, has called for greater adoption of integrated health service models to fast-track the continent’s fight against HIV, Syphilis, and other STIs.
Speaking on the sidelines of the ongoing Triple Elimination Conference 2025, Dr. Buzaalirwa highlighted AHF’s innovative “wellness clinic” model as a practical example of how health systems can integrate services and maximize existing infrastructure to improve disease prevention and care.
“The link between sexually transmitted infections (STIs) and HIV is undeniable,” Dr. Buzaalirwa said. “People with STIs are three times more likely to acquire HIV. Similarly, HIV-positive individuals with untreated STIs transmit the virus more easily due to open sores and immune response reactions.”
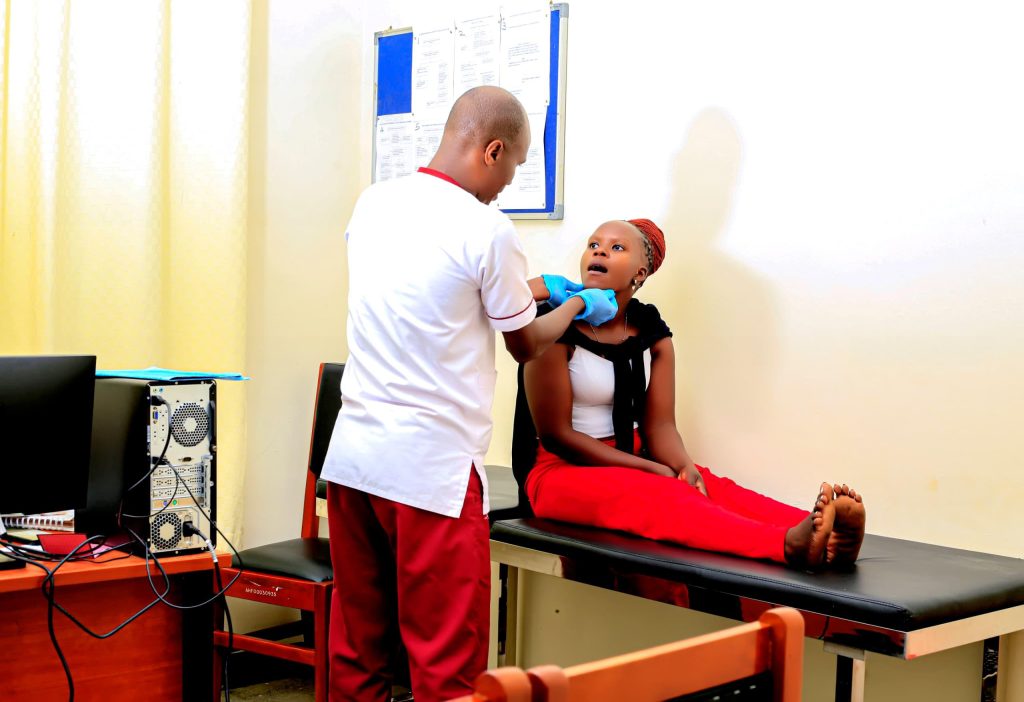
In response, AHF has implemented wellness clinics within its HIV treatment centers to provide STI screening and treatment as part of routine HIV care. The model is simple yet effective—any individual suspecting exposure to an STI can walk into these clinics for screening, counseling, testing, and, where necessary, treatment.
The process begins with an initial screening by a nurse using a standardized risk profile, followed by counseling, lab testing, and immediate access to clinical care based on the results.
According to Dr. Buzaalirwa, this integration has helped identify people who would never have come for HIV testing but are willing to access STI care—leading to a higher detection rate of new HIV cases.
One such clinic, located in Lukaya—a known transit hub for truck drivers and hotspot for commercial sex work—has become a model for targeted interventions in high-risk communities.
However, the program hasn’t been without its challenges. Internally, some healthcare workers have resisted the initiative, viewing it as added workload. AHF has since introduced shift systems to address staffing issues and promote efficiency. Regionally, some countries have been slow to approve wellness clinics, citing regulatory concerns or potential conflicts with other partner organizations.
Diagnostics and testing also present hurdles. Dr. Buzaalirwa pointed to the high cost and limited availability of World Health Organization-approved test kits, such as GeneXpert cartridges, as barriers to scaling up services.
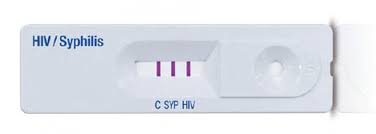
Despite the challenges, she praised the impact of dual test kits—like those that test for both HIV and syphilis in a single sitting—as game-changers in simplifying diagnostics and saving time.
Stigma remains another persistent obstacle. “Many people still fear being associated with STIs or HIV. That fear keeps them away from clinics,” she said. AHF has responded by ensuring confidentiality, accelerating services, and discreet outreach through social media and peer educators. But legal and cultural issues—such as criminalization of sex work and same-sex relationships—continue to deter vulnerable groups from accessing services.
Dr. Buzaalirwa called for urgent policy reviews to enable wider implementation of integrated wellness clinics. “If policymakers, civil society, and implementers come together and embrace this model, we can make significant progress toward eliminating mother-to-child transmission and reducing new infections of HIV, syphilis, and other STI’s,” she emphasized.
As the Triple Elimination Conference concludes, Dr. Buzaalirwa’s message is clear: integration, innovation, and community-centered care are critical to achieving Africa’s public health goals.



